Osteoporosis – Part 2
I heard the word “osteoporosis” for the first time when I was a young girl. I remember seeing my Grandmother one day who was very stooped. I said to my Mom “Boy Grand-mère sure has bad posture”. My mother then told me “She doesn’t have bad posture, she has osteoporosis. She can’t stand upright.” I know today that she likely had at least one or more vertebral fractures in her upper spine due to bone loss. Limited physical activity, poor nutrition and the fact that she had 12 kids (!) likely all contributed to her bone loss.
Fractures
Why is bone loss so serious?
Bone loss can lead to fractures. Fractures can lead to limitations in quality of life and even death. It can be that serious. It certainly isn’t always the case, but the potential for health complications is elevated with bone loss.
Fractures in Osteoporosis
Osteoporotic fractures are often called “fragility fractures” or “low-trauma fractures”. These types of fractures occur when we’re doing something that shouldn’t so easily break a bone. Examples include: sneezing or coughing, a fall from standing height, slipping on ice, tripping, lifting something, etc. 1
There are 3 main areas where we tend to fracture with osteoporosis: the spine, the wrist and the hip. Why? Because these three areas have little or no muscle attachments in the areas that tend to fracture. When we move our muscles, they pull on bones via tendons. This pulling action on the bones causes them to get stronger. If bones do not have muscle/tendon attachments, or very few, they do not get stressed as they need to, to remain strong and build up.
1) Spine:
- Fractures will occur in the vertebral body (see photo below). There are no muscles attached to the body of the vertebrae, therefore there is no mechanical pulling on them. This means that this part of the vertebrae is not stressed and can weaken overtime, leading to bone loss and potential fracture.
- Spinal fractures can lead to loss of height, back pain, stooped posture.
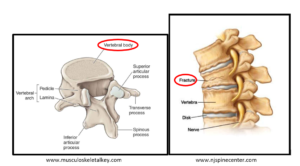
2) Wrist:
- Fractures can more easily happen at the wrist, in particular in the radius bone – the bone in line with the thumb. The distal part of the radius (the end of the bone nearest the thumb), has only 2 small muscles attaching to it. Therefore there is very little mechanical loading and pulling on that end of the bone. We can more easily fracture this bone if we don’t purposefully weight bear on it to strengthen it. This is why simple falls can lead to wrist fractures when normally they shouldn’t.
3) Hip:
- An osteoporotic fracture at the hip generally happens at the neck of the femur (thigh bone). The head of the femur joins the pelvis to form the hip joint. There are no muscles that directly attach to the neck of the femur, therefore there is no direct muscle pulling/loading in that area.
- Hip fractures are very serious as they can lead to death
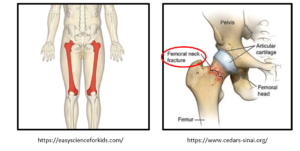
Prevention – Exercise and Nutrition
Exercise:
Physical activity places an increased “load” or “force” on our bones. Let’s remember that bones respond to “loading” or “force” by forming new bone and remodeling the bone to be stronger. Bones NEED to be stimulated by physical activity to maintain their structural competence and strength.1
Osteoporosis Canada has a program called “Too Fit to Fall of Fracture”. It is a series of exercise recommendations for people with osteoporosis or spine fractures. These guidelines are also applicable to those wanting to prevent bone loss (that’s ALL OF US!).
They suggest 4 types of exercise and activity necessary for the management of low trauma fractures and osteoporosis, as well as general bone health:1
1) Strength and Weight-bearing
- Strength Training:
- At least 2 x per week
- Using bodyweight, bands or weights
- Exercises for legs, chest, arms, shoulders and back
- 8-12 reps per exercise
- Examples include: squats, rows, chest presses
- Get STRONG with Lynne with at-home, online strength classes: www.becauseyoucanstrong.ca
- Weight-bearing exercises:
- Definition: Weight-bearing is any activity that one performs on one or both feet, or one or both hands. Weight-bearing is an activity that the skeletal system does against gravity. This can be bodyweight or with the addition of weights. By weight-bearing, the skeletal system adapts to the impact of muscles and body weight and becomes more stable and stronger.
- Since there are bones that have little or no muscle attachments (hip, spine, wrist), we must do weight-bearing exercises to stimulate those bones.
- Examples include: pushups, plank, squats, lunges, walking, running
2) Posture Awareness
-
- Posture: focus on pulling up and preventing slouching. Keep chin slightly tucked, chest up with collar bones open.
- Watch the video called “Maintaining Proper Posture”
3) Balance Exercises
-
- Fall prevention is KEY to preventing fractures. Balance is something that must be worked on everyday. Our ability to balance diminishes if we don’t work on it. Poor balance can lead to falls. Falls can lead to fractures.
- Balance exercises should be done daily for 15-20 minutes.
- Progress from “standing still” exercises to dynamic ones.
- Examples include: tandem stance (heel to toe) or tandem walk, one-leg stand, shift weight from heels to toes, Tai Chi, Essentrics
- Video: https://www.youtube.com/watch?v=ZG0y5iRm0Vk&t=12s
4) Aerobic Physical Activity
-
- At least 150 minutes per week
- Bouts of 10 minutes or longer, moderate to vigorous intensity
- Examples include: brisk walking, dancing, jogging, aerobics
Nutrition:
A well-balanced diet is always a recommendation for overall health. When we think of bones and prevention of osteoporosis, we also need to think about specific requirements, such as calcium and vitamin D.
According to Osteoporosis Canada, Calcium and Vitamin D are essential nutrients for proper bone health. Vitamin D helps to increase the absorption of calcium, ultimately building stronger bones. It also improves the function of muscles, improving your balance and decreasing the likelihood of falls, which can lead to fractures. Among Canadians 40 years of age or older, less than half reported taking calcium and vitamin D supplements.
Bone is a living tissue, that is constantly renewing and repairing itself from everyday wear and tear. Calcium is essential to helping the remodeling process stay balanced. However, like many nutrients, calcium is absorbed less effectively as we age. Studies of older adults show that adequate calcium intake can slow bone loss and reduce the risk of fracture.2
- Adults between 19-50 years of age, including pregnant or breast feeding women, require 1,000 mg of calcium daily
- Those over 50 require 1,200 mg calcium daily
- Try the Calcium Calculator to see if you’re getting enough of this mineral
- Read this list of foods rich in Calcium.
Experts recommend that all Canadian adults take a vitamin D supplement (specifically, vitamin D3 or cholecalciferol) year-round. This is the most common type of vitamin D found in supplements in Canada.2
- Healthy adults between 19-50 years of age, including pregnant or breastfeeding women, require 400-1,000 IU daily;
- Those over 50 or younger adults at high risk (with osteoporosis, multiple fractures, or conditions affecting vitamin D absorption) should receive 800-2,000 IU daily.
- Read this list of foods that are high in vitamin D
Final Thoughts
Let’s not wait till we have a diagnosis of osteopenia or osteoporosis to exercise and eat well. Start moving NOW. Start making better food choices NOW. Let’s keep our bones strong and make them even stronger with daily activity and good nutrition. Let’s age with strength, vitality and confidence. Because you can.
References:
1 – Bonefit manual, www.bonefit.ca


